2024 Pharmacy Benefits
Employees who enroll in a medical plan at Dartmouth College are automatically enrolled in a pharmacy plan offered through Express Scripts.
Contact Express Scripts
- 877-788-5766
- http://www.express-scripts.com/Dartmouth
What is changing in 2024?
-
Plan Design - There are no plan design changes or copay cost changes planned for calendar year 2024.
Other Important Open Enrollment Information
-
Costs/Tier Changes - Some medications are scheduled to change in cost and/or tier level on January 1st, so it is important to check the costs of your medications by using the price a medication tool found at http://www.express-scripts.com/Dartmouth. Select a medical plan, and then select the price a medication option. Most members impacted by a change in cost/tier level will be notified in writing by Express Scripts, so please watch your mail for these notifications.
Create an Account
Prior to enrollment and creating your account, you may use the http://www.express-scripts.com/Dartmouth link to obtain costs of your individual medications to assist with medical plan choice. You can also find preferred drug lists, participating pharmacies and more.
Once your coverage starts, you can set up your own personal account where you can order medications online, monitor refills, check prior authorizations, find additional savings and more. To set up your account, go to http://www.express-scripts.com/Dartmouth, click HOW TO ENROLL at the top and then click on REGISTER to create your own personal account. Family members over age 18 may also create their own personal accounts and manage their own prescriptions.
Use the Express Scripts Mobile App to store your ID Card, access your medications at a moment's notice, see when refills are needed, and manage your mail order refills.
Eligibility and Enrollment
All benefit eligible employees may enroll themselves and their eligible family members in one of Dartmouth's three medical plans available through Cigna. Pharmacy coverage comes with your Cigna health plan, and is provided by Express Scripts. You do not need to enroll in a pharmacy plan, as coverage is determined by the medical plan that you choose.
New Hires may enroll in medical insurance (with pharmacy coverage) within their first 30 days of employment, otherwise existing employees may enroll during the annual open enrollment period held each fall for a January 1st start date. Some IRS eligible life events causing a drop in external medical insurance will allow for enrollment in a medical plan for yourself and/or your dependents through Dartmouth. Life events must be completed in the FlexOnline system within 30 days of the event.
ID Cards
Please allow 7 to 14 days from new hire enrollment for new ID cards to arrive in the mail. You will receive an ID card for each covered member of your family. If you lose your ID card, please contact Express Scripts at the number above, or you may access a copy through the Express Scripts mobile app.
Cost of Medications
Preventive Medications
Certain preventive prescriptions are offered at no cost to members enrolled in the HDHP medical plan. A comprehensive list of these prescriptions can be found at www.express-scripts.com/Dartmouth.
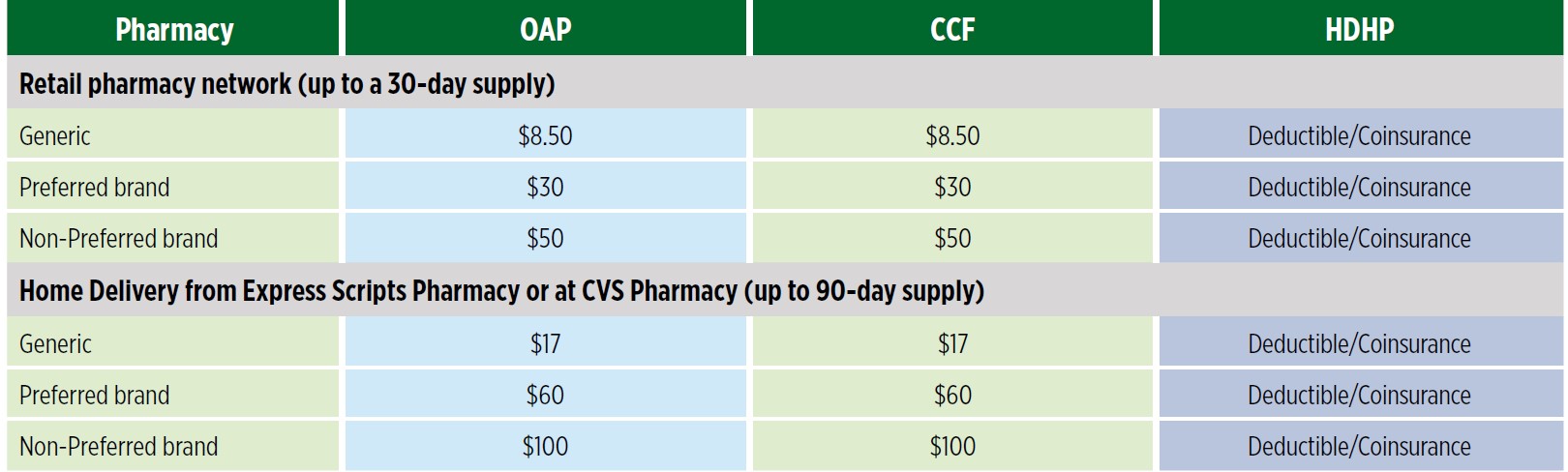
Tiered Drug Pricing
Many preferred and non-preferred brand medications have less expensive generic alternatives. Talk to your doctor to see if there is a generic version of your existing medication and if so, whether it might be a viable option for you.
Price a Medication Tool
It is important to understand your regular out-of-pocket prescription costs prior to enrolling in a medical/pharmacy plan. High-cost medications can often negate the savings of a low cost High Deductible Health Plan. No one wants a surprise at the pharmacy. To determine the cost of your regular medications please use the prescription drug cost calculator from Express Scripts at www.express-scripts.com/Dartmouth. Please also note the PillarRx section below
We also encourage you to share this tool with your provider when they are reviewing new medications for you. You may want to try a lower cost generic option prior to starting a higher cost preferred or non-preferred brand option.
Specialty Medications
See the PillarRx section below for information and costs when filling higher cost specialty medications.
90-Day Prescriptions/Mail Order
When you fill a 90-day maintenance medication through Express Scripts mail order or at a CVS retail pharmacy, you will only be charged the cost of a 60-day fill. Refer to the tiered drug pricing chart shown above. 90-day prescriptions can also be filled through Dick's House pharmacy on campus, but you will pay the equivalent of three 30-day supplies. 90-day fills are not available through other pharmacy locations.
Express Scripts Mail Order Form
Costs when filling odd amounts
Standard prescriptions are filled in 30-day increments; 30-day, 60-day and 90-day fills. When purchasing prescriptions in odd amounts you may pay more per dose. For example, a 10-day fill may cost the same as a 30-day supply and a 45-day fill may cost the same as a 60-day supply. Use the Express Scripts cost tool to see how odd fill amounts will impact your out-of-pocket cost. You may want to work with your provider to see if they can write a per-day amount that will be more cost effective for you.
What Medications are Covered under the plans.
The National Preferred Formulary
A formulary is a list of medications covered under your pharmacy plan which provides a guide for you and your prescriber, to help you choose the most clinically appropriate and cost-effective medications available. It is recommended that you and your prescriber refer to the Formulary list when determining which medication may be best for you.
- Access the Express Scripts Formulary and select a plan to check your medication coverage.
- Periodically, medications can change tier levels or be removed from the list of covered medications (formulary).
- Always take notice of communications from your insurance venders for important notices and to avoid potential disruption.
- If you are ever affected by a formulary change, you will be notified through US mail, in advance by Express Scripts, and are encouraged to have a conversation with your prescriber.
PillarRx
Dartmouth works with PillarRx to assist employees and family members who take specialty
medications for complex or chronic medical conditions. If you or your covered spouse
or dependent take a specialty medication through Accredo for which the Copay Assistance
program is available, you will receive information directly from PillarRx. Enrollment
is mandatory in this program if you take one of these medications. If you find the
Express Scripts price a medication tool is bringing back a high cost for your specialty
medication, it may be worth contacting PillarRx at the number below to see if the
medication is eligible for copay assistance under the PillarRx program. Most eligible medications are covered at a $0.00 cost to the member. For more information please click here.
- Manufacturer coupons do not apply toward your annual deductible on the HDHP.
- Reach PillarRx at 636-614-3126
Pharmacy coupons
Some prescription drug coupons cannot be used in conjunction with Dartmouth’s prescription
drug plans.
Please check with your pharmacist prior to using a coupon.
Find a Provider
Express Scripts has a broad retail network of more than 56,000 participating pharmacies nationwide, including:
- Independent pharmacies
- Chain pharmacies such as CVS and Walgreens
To find pharmacies within your area that are in-network go to www.express-scripts.com/Dartmouth click on any of the three medical plans, and then select FIND A PHARMACY.
Filling a Prescription
Your Express Scripts (ESI) prescription ID card must be presented when filling a prescription. Do not use your Cigna medical ID card when filling prescriptions at the pharmacy.
Mail Order Pharmacy
For some maintenance medications, you may find that using Express Scripts Mail Order service for 90-day prescriptions is a more cost-effective way of getting your medications. Use the Express Scripts price a medication tool to compare costs through mail order and retail pharmacies.
Retail Pharmacies
Prescription drugs must be paid for at the time of pickup. If you pay the full cost of a prescription out of pocket, you will only be reimbursed at the Express Scripts "allowed" amount. Most pharmacies will reimburse the funds if you return within 14 days with your pharmacy ID card and original receipt. Please talk to your pharmacist about your options prior to paying the full out-of-pocket cost. If you have an urgent situation, please contact the benefits office at 603-646-3588.
If you do pay full cost for a prescription, then you will need to submit a claim to Express Scripts, using the Express Scripts Claim Form.
Switching Plans
Whenever possible, we recommend filling a 90-day supply of all important or maintenance medications prior to switching employment or insurance coverage(s).
Prior Authorizations
To ensure you’re receiving the treatment plan that is right for you, there are some medications that require prior authorization before they can be filled at the pharmacy. Prior authorization is an approval from your doctor, confirming that the medication prescribed is both appropriate for your condition and cost effective for you. In these cases, the pharmacy will not fill your prescription until the prior authorization has been approved.
Physician's Prior Authorization line: 800-417-8164 option 3
A prior authorization is facilitated by your doctor through a four-step process:
- Inquiry Received
- Outreach to Prescriber
- In Review (This typically takes 24-48 hours.)
- Approved, Denied, Withdrawn or Other
Leaving Dartmouth
Your pharmacy benefits end when your medical benefits end. If you continue your Cigna medical coverage under your COBRA rights, then your pharmacy coverage will also continue. If you do not continue your Cigna medical coverage under COBRA, then your pharmacy coverage will end on the last day of the month in which you are benefits eligible with Dartmouth.
Transitioning to other coverage
If you take regular maintenance medications, we highly encourage you to fill a 30 to 90 day prescription just prior to your coverage ending here at Dartmouth. This will allow time for your new coverage to be established before having to request your next refill.
What If I Need a Prescription Prior to Receiving/Returning My COBRA packet?
Prescription drugs must be paid out of pocket and will only be reimbursed at the Express Scripts "allowed" amount. However, most pharmacies will reimburse the overpayment, if you return within 14 days with your pharmacy ID number and original receipt. Please speak with your pharmacy about their process in these cases and what they will allow. If you have an urgent situation, please contact the benefits office at 603-646-3588.
